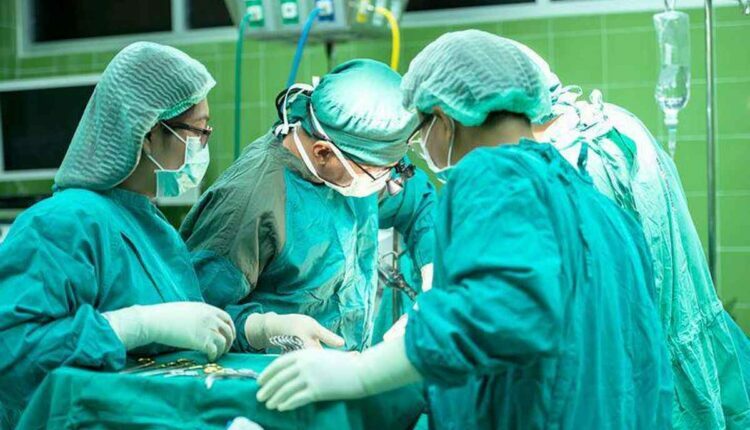
To comprehend how surgical procedures aid the actual grossly overweight person to lessen their body fat, it helps to very first understand the digestive process which is responsible for handling the food put into effect.
Once the food is chewed and swallowed, it’s coming through the digestive tract, where digestive enzymes and digestive juices will certainly break it down and permit our systems to absorb the actual nutrients and calories. Within the stomach, which can hold up to a few pints of material, the elimination continues with the help of strong gastric acids. From there it moves to the duodenum, and the digestive course of action speeds up through the addition of fiel and pancreatic juices.
Really here, our body absorbs the majority of iron and calcium supplements in the foods we try to eat. The final part of the digestive course of action takes place in the 20 legs of the small intestine, typically the jejunum and the ileum, exactly where calorie and nutrient compression is completed, and just about any unused particles of foodstuff are then shunted in the large intestine for reduction.
Weight loss procedures involve breaking, or in some way circumventing the total digestive process. They cover anything from the simple reduction of the volume you can eat, to major bypasses in the digestive tract. To qualify for most of these surgeries, a person needs to be termed “morbidly obese”, weighing at least 100 pounds. over the appropriate weight for his or her height and general physiology.
Gastric Bypass
In the middle of the 1960s, Dr . Edward Electronic. Mason discovered that women who experienced undergoing partial stomach elimination as the result of peptic ulcers failed to gain weight afterward. Using this observation, grew the demo use of stapling across the top of the stomach, to reduce its real capacity to about three tablespoons. The actual stomach filled quickly and finally emptied into the lower part, completing the digestive procedure in the normal way.
Through the years, the surgery evolved into what is now known as the actual Roux-en-y Gastric Bypass. Rather than partitioning the stomach, it really is divided and separated through the rest, with staples. The small intestine is then cut approximately 18″ below the abdomen, and attached to the “new”, small stomach. Smaller dinners are then eaten, plus the digested food moves into the lower part of the bowel. While weight-loss surgeries are considered overall, this is considered one of several safest, offering long-term operations of obesity.
Gastric Fixing
A procedure that produces this can be the same results as the abdomen stapling/bypass and is also classed being a “restrictive” surgery. The first surgical procedures involved a non-flexing strap placed around the upper portion of the stomach, below the esophagus, generating an hourglass-shaped abdomen, the upper portion being diminished to the same 3-6 oz capacity.
As technologies superior, the band became way more versatile, incorporating an inflatable go up, which when triggered by any reservoir placed in the belly, was capable of inflating to take down the size of the stoma or deflating to expand it. Laparoscopic surgery implies smaller scars and less intrusion of the digestive tract.
Biliopancreatic Feint
A combination of the gastric sidestep, and Roux-en-y re-structuring, will bypass a significant section of the tiny intestine, thereby creating the chances of malabsorption. The abdominal is reduced in size, in addition to an extended Roux-en-y anastomosis is definitely attached to the smaller stomach, in addition to lower down on the small interact with than is normal.
This licenses the patient to eat larger volumes, but still achieve weight loss by malabsorption. Professor Nicola Scopinaro, University of Genoa, France, developed the technique, in addition to last year published the first good results. They showed the normal 72% loss of excess body volume, maintained over 18 several years, the best long-term results of almost any bariatric surgical procedure, to date.
BPD patients require lifelong follow-ups to monitor calcium and vitamin supplements intake. The advantages of being able to feed on more and still lose weight, are usually countered by loose or perhaps foul-smelling stools, flatus, stomal ulcers, and achievable protein malnutrition.
Jejuno-Ileal Sidestep
One of the first weight loss procedures for the grossly obese was developed almost 50 years ago, a strictly malabsorptive way of reducing weight, and preventing acquire. The jejunoileal bypass lowered the lower digestive tract to a minuscule 18″ of small interact with, from the natural 20 toes, a critical difference when it came to ingestion of calories and nutritional value.
In the end-to-end method, the top of the intestine was severed under the stomach and re-attached into the small intestine much lower decrease, which had also been cut, thereby “cutting out”, the vast majority of the intestine. Malabsorption of carbo, protein, lipids, minerals, and vitamins, ended in a variation, the end-to-side bypass, which took the bottom of the upper portion, in addition to attaching it to the side with the lower portion, without cutting at that point.
Reflux of a bowel contents into the nonfunctioning higher portion of the small bowel, triggered more absorption of essential goodness, but also less weight loss, and also increased weight gain, post-surgery. Because of the bypass, fatty acids are usually dumped in the colon, creating an irritation that causes water and also electrolytes to flood the particular bowel, ending in long-term diarrhea. The bile sodium pool necessary for keeping cholesterol in solution is reduced simply by malabsorption and loss by means of stool.
As a consequence, cholesterol attention in the gall bladder springs up, increasing the risk of stones. Many vitamin losses are an important concern and may result in heel bone thinning, pain and rupture. Approximately one-third of affected individuals experience an adjustment inside size and thickness with the remaining active small interact, which increases the absorption connected with nutrients, and balances out weight loss.
However, over the long run, all patients undergoing that bypass are susceptible to hepatic cirrhosis. In the early 1980s, one study exhibited that approximately 20% of those who had undergone JIB, had a necessary conversion to another bypass alternate. The procedure has since recently been largely abandoned, as possessing too many risk factors.
Although surgical methods of reducing weight are usually valuable to the morbidly overweight, they are not without risks. Individuals may require more bed relaxation post-surgery, resulting in an increased potential for blood clots. Pain might also cause reduced depth regarding breathing, and complications like pneumonia.
Before undergoing virtually any fat/weight reduction surgery, a new severely overweight person should thoroughly understand the benefits in addition to risks and must make a consignment to their future health. Having a small stomach is not going to stop often the chronic sugar-snacker, from “grazing” on high calorie treats.
Nor does a steady method to obtain pop, concentrated sweet tasty mix, and milkshakes can help calorie intake. With some bypass surgical practices, certain foods can aggravate side effects that need not be that intense, if common sense diets usually are adhered to. Surgery can be a “shortcut” to weight loss, but it might also reduce your enjoyment of life when you are unable to adhere to the sessions that go with it.
Read also: Strava Apple Watch Current Pace – 5 Reasons Why One Should Buy a Physical fitness Tracker