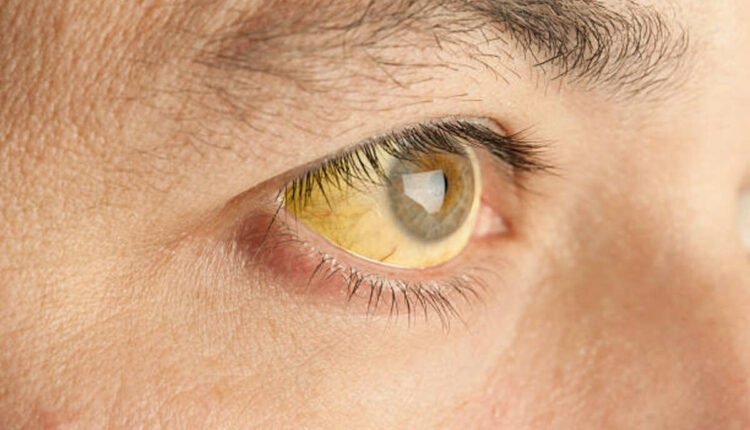
Jaundice is caused by the break up of red blood cells in the baby’s blood. It is caused by an enzyme called G6PD, a deficiency of which can lead to jaundice. People with African heritage are the most likely to have this disorder. Genetic problems can also cause jaundice.
Pathologic jaundice
Pathologic jaundice is a condition that is caused by excessive breakdown of red blood cells. Other causes include disorders of bilirubin metabolism. Premature birth and trauma to the GI tract may also cause jaundice. Pathologic jaundice can be temporary or life-threatening. Fortunately, prompt treatment can prevent most complications.
Physiologic jaundice in newborns usually begins around two days of age and peaks by three to five days. Pathologic jaundice is characterized by an increased bilirubin level and requires medical intervention to remove it. In addition, pathologic jaundice can be a symptom of other illnesses, including sepsis and a urinary tract infection.
Treatments for pathologic jaundice often include phototherapy and blood exchange transfusion. These treatments reduce bilirubin levels and reduce the risk of kernicterus. However, these treatments cannot cure pathologic jaundice completely. Ultimately, a child with pathologic jaundice needs a different type of treatment to prevent kernicterus.
The main aim of treatment for pathologic jaundice is to treat the underlying disorder. Most physiologic jaundice cases are not considered clinically significant and resolve within one week. Frequent formula feeding can reduce the incidence of pathologic jaundice and minimize enterohepatic circulation of bilirubin. The type of formula used in feeding does not seem to be a factor in increasing bilirubin excretion.
The primary treatment for pathologic jaundice is phototherapy, a light therapy. This procedure uses high-intensity light of the right wavelength to change the bilirubin pigment into a nontoxic form that can be excreted in the urine. Phototherapy also helps keep the baby hydrated while addressing other underlying problems. In some cases, an exchange transfusion is needed to remove bilirubin from the baby’s bloodstream.
Genetic problems that cause red blood cells to break apart
People with thalassemias have thin, fragile red blood cells. This disease is caused by gene changes affecting red blood cell membrane proteins. As a result, the cells become damaged and break apart. This reduces the number of RBCs in the body. Affected individuals can develop anemia or jaundice as a result of the disease. They may also experience a decrease in hemoglobin levels.
When red blood cells break apart, they can leak bilirubin into the blood, which can lead to jaundice, dark urine, and even gallstones. People with this disease can also experience extreme fatigue, paleness, headaches, and dizziness. These symptoms can make it difficult for people to eat or sleep.
People with hemolytic anemia should stay out of cold weather and wear warm clothes. They should also try to keep their homes warmer. This condition can either be inherited or acquired. In inherited hemolytic anemia, the red blood cells break apart before the bone marrow can replace them. Some people with this condition may also have a heart murmur.
Sickle cell disease is another inherited disease causing abnormal red blood cells. The hemoglobin in sickle cells is made of a different type of hemoglobin than usual. As a result, the red blood cells are stiff and rigid, which blocks oxygen flow to tissues. This can cause pain and damage to organs. In severe cases, patients may develop heart failure or kidney failure. The disease does not cause symptoms in the early stages but can lead to early death.
Treatment options
There are several treatment options for jaundice. Generally, phototherapy is the first choice. However, if that fails, intravenous immunoglobulin may be given. It works by diluting maternal antibodies and bilirubin. This procedure is often done in the neonatal intensive care unit.
Depending on the severity and cause of the condition, medications or lifestyle changes may be recommended. If the condition results from liver disease, surgery may be necessary. In some cases, an infection may damage the liver and require a liver transplant. However, if the condition is mild and self-limited, there are other treatment options for jaundice.
There are several causes of jaundice. These include liver diseases, autoimmune disorders, drugs, and infections. Infections can cause jaundice in babies. Some are benign, such as herpes simplex. More serious ones include sepsis and galactosemia. Several genetic diseases can cause jaundice in children. The good news is that most of them are pretty rare. Premature babies are also at an increased risk for jaundice.
If you suspect your baby may have jaundice, the first step is to visit the pediatrician. The pediatrician will help you decide on the best treatment. In mild cases, exposing your baby to sunlight daily and properly feeding the child can help reduce the symptoms of jaundice. In severe cases, bilirubin levels may need to be checked.